 Because HNC is a heterogeneous disease entity with tumours originating from the nasopharynx, oropharynx, hypopharynx, larynx and oral cavity, tumour location may influence the prognosis and survival of HNC. In the present study, heterogeneity in the OS analysis may have resulted from the inclusion of all subsites of HNC. Subgroup analyses were conducted to reduce the potential confounding factors. 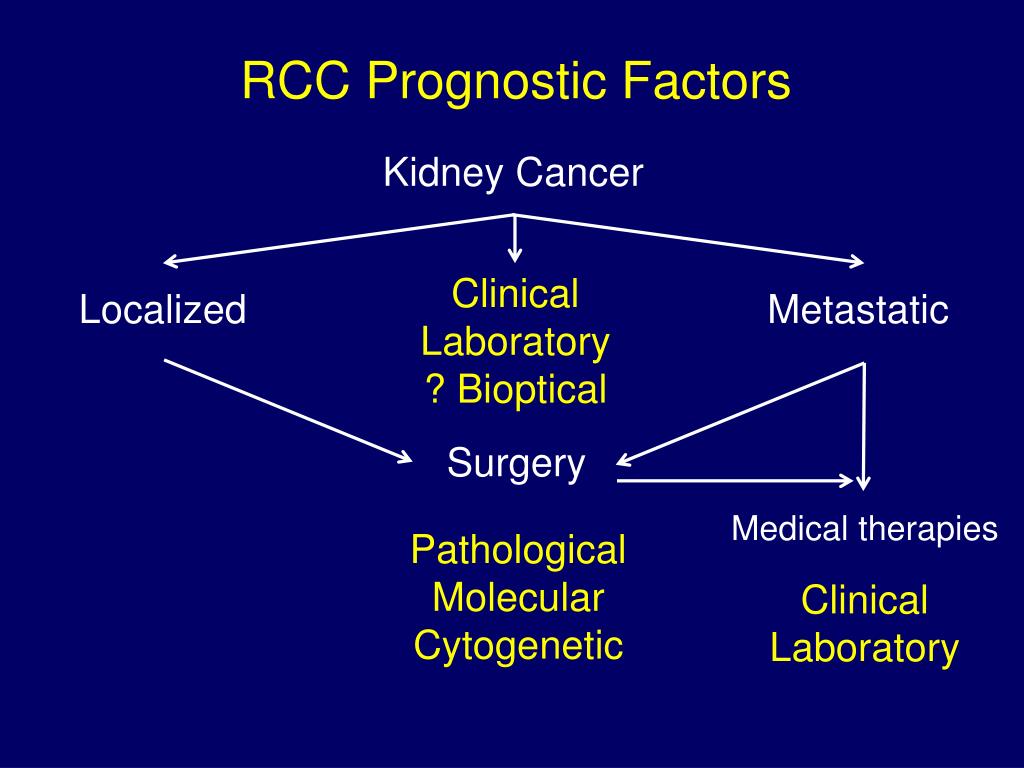 
Thus, we performed this meta-analysis by pooling the related literature to quantify the prognostic value of PNI on survival outcomes in patients with HNC. While the assessment of some haematological biomarkers involves expensive testing, the PNI is a readily available and cost-effective marker in the pretreatment evaluation of patients via blood tests. Therefore, conducting a comprehensive meta-analysis may provide evidence supporting clinical practice and the formation of clear clinical guidelines for HNC. However, no HNC patients were included in this meta-analysis. A meta-analysis investigated the relationship between PNI and tumour survival through 14 published studies and found that a low PNI level was associated with poor overall survival (OS) in terms of tumour type, surgical condition, cut-off value, sample size and area 16. Several studies conducted PNI as an independent prognostic biomarker in cancers, including oesophageal squamous cell carcinoma, small or non-small-cell lung cancer, pancreatic cancer, gastric cancer and colorectal cancer 9, 10, 11, 12, 13, 14, 15. The prognostic nutritional index (PNI) incorporating serum albumin level and peripheral blood lymphocyte count serves as an indicator of systemic inflammation and host nutritional status. Identification of precise and available prognostic indicators may optimize the management of patients suffering from HNC. Accumulated studies have shown that many inflammation-based scores, including the neutrophil-to-lymphocyte ratio, Glasgow prognostic score, lymphocyte-to-monocyte ratio, platelet-to-lymphocyte ratio, and C-reactive protein to albumin ratio, are associated with cancer survival and prognosis 7, 8. Increased evidence has shown that host immunity and systemic inflammation play an important role in cancer angiogenesis and progression, although the exact pathogenesis is not thoroughly understood 5, 6. Therefore, understanding tumour carcinogenesis and identifying available serum biomarkers of HNC could contribute to personalized treatment with better prognosis prediction and patient stratification 3, 4. Despite advances in multidisciplinary management and aggressive treatment in HNC, the prognosis is still unsatisfactory, and the survival outcomes of patients with the same tumour-node-metastasis (TNM) stage usually vary 2. Surgical resection combined with or without adjuvant therapy based on clinical and pathological risk factors and radiotherapy with or without chemotherapy remain the standard treatment for HNC. Multidisciplinary approach to patients with HNC at different stage and situation was based on institution guidelines, while two main strategies were widely performed. 
More than 400,000 people died of HNC in 2018, and 800,000 cases were newly diagnosed each year 1. Head and neck cancer (HNC), which includes several malignancies arising from the oral cavity, nasopharynx, oropharynx, hypopharynx and larynx, is an important issue of public health worldwide. Elevated pretreatment PNI is correlated with a superior prognosis in HNC patients and could be used asĪ biomarker in clinical practice for prognosis prediction and treatment stratification. Furthermore, low pretreatment PNI was correlated with poor OS despite variations in the cancer site, sample size, PNI cut-off value, analysis method (multivariate analysis or univariate analysis) and treatment modality in subgroup analysis. A total of 7815 HNC patients from 14 eligible studies were involved. A random-effects model was used to calculate the pooled hazard ratios (pHRs) and corresponding 95% confidence intervals (CIs). Overall survival (OS), progression-free survival (PFS), disease-specific survival (DSS), disease-free survival (DFS) and distant metastasis-free survival (DMFS) data were collected and evaluated. A systematic search through internet databases including PubMed, Embase, and Cochrane Library for qualified studies estimating the association of PNI with HNC patient survival was performed. 
We conducted a meta-analysis to assess the predictive value of PNI in HNC patients. The predictive value of the pretreatment prognostic nutritional index (PNI) for head and neck cancer (HNC) remains controversial. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
